About the Trial
The “StOP?-protocol” research project aims to improve communication during surgical operations to contribute to improved patient outcomes. In a first study (Tschan et al., 2022) the StOP?-Protocol was shown to be effective in reducing mortality, length of stay, and unplanned reoperation (press information). We now will test these effects in a randomized controlled trial.
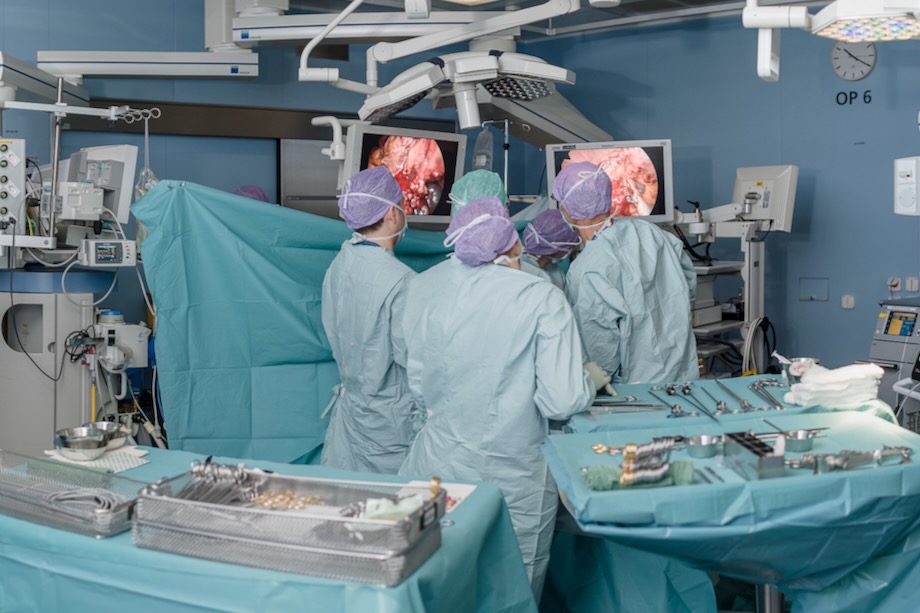
Effective communication within the surgical team has a positive effect on patient outcomes
Worldwide, about 313 million operations are performed each year and unfortunately, 4.2 million people are estimated to die within 30 days after their operation. We therefore need effective interventions to reduce mortality and other complications after surgery. Given that more than 1.1 million surgical procedures are performed annually in a population of 8.6 million inhabitants in Switzerland, the intervention tested in this trial has a tremendous potential to improve patients’ life undergoing surgery.
Outcomes of operations not only depend on patient characteristics and the expertise of the surgeons, but also depend to a great extent on good intraoperative communication and teamwork. In the operating room, surgeons, anesthetists as well as scrub and circulating nurses have to cooperate closely, and all members of the surgical team need to be “on the same page” during the whole operation. Earlier studies showed that effective communication within the surgical team can have a positive effect on patient outcomes. Although most surgical teams use the WHO checklist before starting the operation to exchange information about the patient, there are no tools that ensure communication during the operation within the whole surgical team.
The StOP?- protocol structures and fosters communication during an operation
The current study introduces a communication protocol – named StOP?-protocol – that fills this critical gap. The StOP?-protocol fosters the exchange of information during the surgical procedure in a way that
- is specific enough to ensure that important information is exchanged.
- is flexible enough to ensure that the information exchanged is relevant in light of the development of the specific operation.
- does not disrupt the flow of the operation.
The StOP?-protocol is a short intraoperative briefing within the team present in the operating room and it is initiated and led by the responsible surgeon. It takes typically between 30 and 90 seconds.
All team members present in the operating room are informed:
- about the progress of the surgery (Status)
- the next steps and proximal goals (Objectives)
- possible problems (Problems)
- are encouraged to voice their observations and ask questions (?)
This protocol thereby promotes that the entire team is informed about the progress of the procedure while simultaneously engaging all persons present and promoting feedback.
The StOP?-protocol builds on the results of a previous study and has the potential to improve the outcome of operations
The beneficial effect of the StOP?-protocol on patient outcomes was observed in a previous study that showed effects on mortality, reoperations and length of stay. While the first study was performed using a before-after design, included only four hospitals and concentrated on a limited range of surgeries, a randomized controlled trial is now needed to increase and extend the level of evidence. Therefore, an interventional study was designed focusing on clinical outcomes based on inputs from an advisory board including patients and policy makers. In this multicentric clinical study, individual surgeons from different surgical specialties are randomized either to the control group or to be trained in StOP?-protocol use. The control group represents the local standard of care that may include other interventions such as checklists or team trainings.
Expected results will reveal if clinical outcomes can be improved by addressing team behavior during the performance of complex procedures. In particular, the study has the potential to provide evidence that a short and inexpensive intraoperative briefing may reduce mortality, morbidity as well as patient-reported outcomes after surgery.